Who we help
Members
We help patients access medications that are not covered by their plan or that come with high out-of-pocket costs. Our dedicated care coordinators simplify the process by identifying available programs, managing paperwork, scheduling refills, and ensuring patients receive the support they need.
Partners
We support consultants, brokers, and advisors with a proven program that helps clients save on prescription costs while improving member satisfaction.
Employers
We help self-funded health plans control their specialty drug costs—while making over 300 medications more accessible to your members.
URAC certified
URAC is the independent leader in promoting health care quality and patient safety through renowned accreditation programs.
URAC’s accreditation process validates compliance with nationally recognized health care standards and supports improvements and innovation in care management and service delivery for the long term.

The problem with
specialty drug costs
%
Of drug spend is driven by 5% of members
%
Annual price inflation
%
Of total drug spend is specialty
How we help

We educate members on affordable alternatives
When a health plan is unable to cover certain high-cost drugs, we support members by helping them apply for Manufacturer Programs, exploring alternative savings options, and connecting them with certified vendors to provide access to affordable medications.

We simplify a complex process
Navigating the process of applying for medication assistance can be daunting. We support patients every step of the way—helping gather necessary documentation, complete required form forms, and ensure the deadlines are met.

We never charge members
Our services are free to patients. We’re paid by the plan sponsor to serve as an advocate and resource.
Our technology
We’ve invested in the future of health with our own customized solution for gaining deep insight into the patient service journey.
By tracking referrals, benefits, and treatment plans, we can help you ensure quality care for your members and a positive experience.
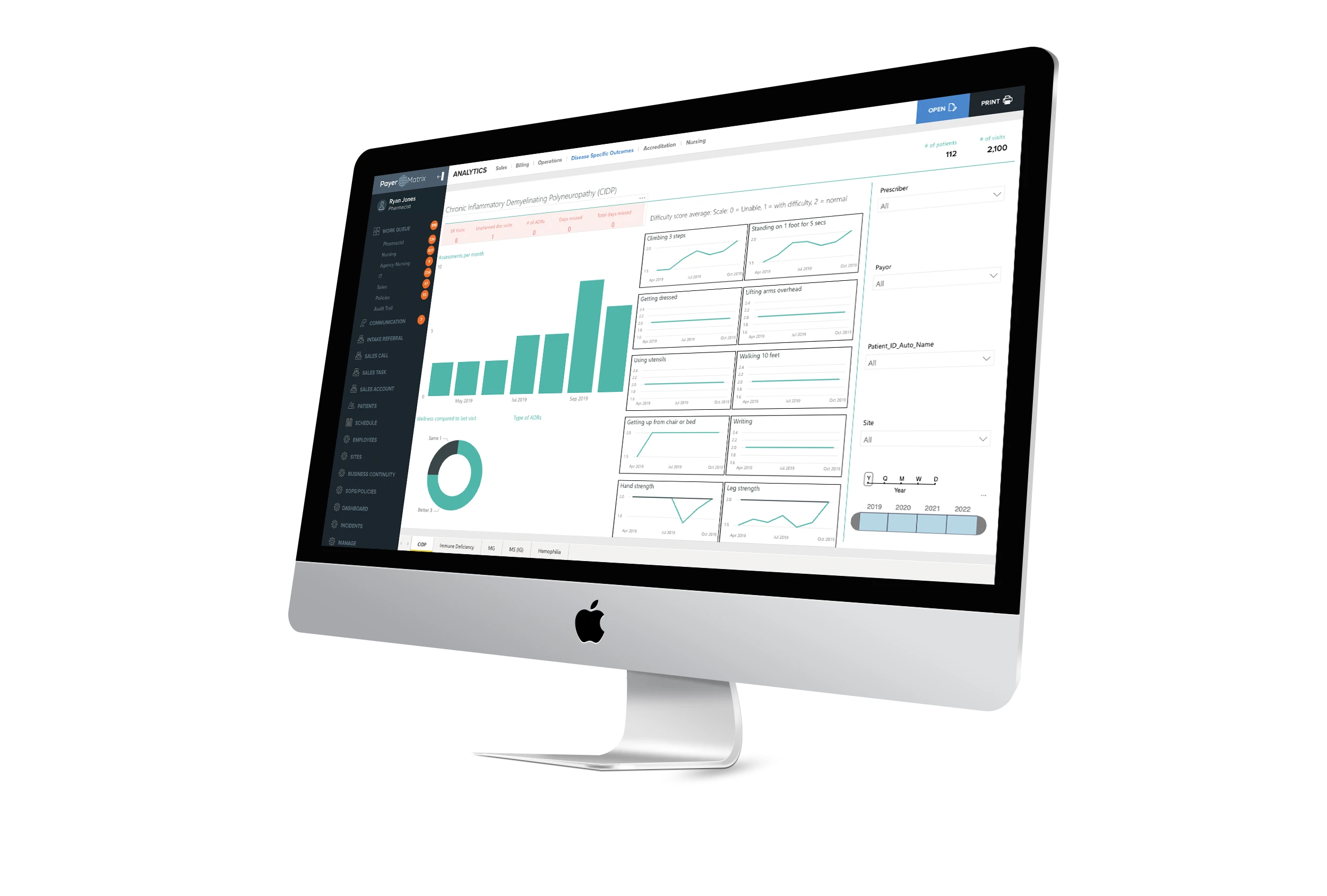

Dashboard analytics
How is your team performing? How much of a drug has been dispensed this past month? We can tell you.

Workflow management
By bringing your workflow into Payer Matrix, we can help you learn where to optimize and improve.
The specialty drug dilemma
We identified a problem facing employers and patients alike, and sought a way to save money while still providing quality care.
What people are saying
When I first came to Payer Matrix, I was really unsure, but after working with my care consultant I couldn’t believe how much they were able to save me. Would recommend!
Member
I spoke to so many insurers and providers trying to understand what was available to me. Payer Matrix talked to me and came up with a comprehensive strategy and delivered best care I could ask for.
Member
When we first started working with Payer Matrix, we saw an immediate return on investment with their analytics and insight into our workflow.
CEO
Contact

Our locations
Media, PA (HQ)
Plano, TX
Overland Park, KS
Deerfield Beach, FL
Office hours
9 AM - 7:30 PM EST
Phone
877-305-6202
Fax
484-494-6670


